Considerable attention has been paid to whether or not changes in the weather may stop the spread of the COVID-19 coronavirus pandemic. Berkeley Earth has conducted a brief review of how the virus has been spreading in comparison to the weather conditions across various locations during the previous months. The most significant early spread occurred in countries with relatively cool temperatures, though this may have been a coincidence. More recently, COVID-19 has also established itself in warmer conditions.
It is our conclusion that warming weather is unlikely to stop the spread of the pandemic. Warm, sunny weather may have some limited impact on the rate of spread, but in the absence of strong interventions, the pandemic is likely to continue spreading through the summer months in most parts of the world. The following brief report provides the justification for that conclusion.
Introduction
It is widely recognized that influenza, i.e. “the flu”, is seasonal. Incidence of the flu increases during the cold season, with a northern hemisphere peak typically during December to February. The reasons for this are not wholly understood but are believed to involve a combination of both physical factors affecting the durability of the virus and social factors relating to humans clustering indoors during cold weather. In addition to influenza, many other widely-occurring viruses exhibit some degree of seasonality, though not all peak at the same time of the year as influenza.
It has been widely hoped that the transition to warmer weather during the Northern Hemisphere months will either slow or stop the spread of COVID-19 in the Northern Hemisphere.
In consideration of this possibility, there have already been several academic preprints released.
In support of a seasonal effect on COVID-19:
- Alvarez-Ramirez and Meraz (2020) Role of meteorological temperature and relative humidity in the January-February 2020 propagation of 2019-nCoV in Wuhan, China. medRxiv 2020.03.19.20039164; doi: https://doi.org/10.1101/2020.03.19.20039164
- Araujo and Naimi (2020) Spread of SARS-CoV-2 Coronavirus likely to be constrained by climate. medRxiv 2020.03.12.20034728; doi: https://doi.org/10.1101/2020.03.12.20034728
- Bannister-Tyrrell et al (2020) Preliminary evidence that higher temperatures are associated with lower incidence of COVID-19, for cases reported globally up to 29th February 2020. medRxiv 2020.03.18.20036731; doi: https://doi.org/10.1101/2020.03.18.20036731
- Bukhari and Yusuf (2020) Will Coronavirus Pandemic Diminish by Summer? http://dx.doi.org/10.2139/ssrn.3556998
- Carleton and Meng (2020) Causal empirical estimates suggest COVID-19 transmission rates are highly seasonal. Preprint.
- Chen et al (2020) Roles of meteorological conditions in COVID-19 transmission on a worldwide scale. medRxiv 2020.03.16.20037168; doi: https://doi.org/10.1101/2020.03.16.20037168
- Ficetola and Rubolini (2020) Climate affects global patterns of COVID-19 early outbreak dynamics. medRxiv 2020.03.23.20040501; doi: https://doi.org/10.1101/2020.03.23.20040501
- Ma et al (2020) Effects of temperature variation and humidity on the mortality of COVID-19 in Wuhan. medRxiv 2020.03.15.20036426; doi: https://doi.org/10.1101/2020.03.15.20036426
- Sajadi et al. (2020) Temperature, humidity and latitude analysis to predict potential spread and seasonality for COVID-19. doi: http://dx.doi.org/10.2139/ssrn.3550308
- Wang et al (2020) High temperature and high humidity reduce the transmission of COVID-19. doi: http://dx.doi.org/10.2139/ssrn.3551767
- Wang et al (2020) Temperature significant change COVID-19 Transmission in 429 cities. medRxiv 2020.02.22.20025791; doi: https://doi.org/10.1101/2020.02.22.20025791
In opposition to a strong seasonal effect:
- O’Reilly et al. (2020) Effective transmission across the globe: the role of climate in COVID-19 mitigation strategies. https://cmmid.github.io/topics/covid19/current-patterns-transmission/role-of-climate.html
- Tahira Jamil, Intikhab Syed Alam, Takashi Gojobori, Carlos Duarte (2020) No Evidence for Temperature-Dependence of the COVID-19. https://doi.org/10.1101/2020.03.29.20046706
In addition, there are likely other papers that we have overlooked.
Temperature vs. Case Numbers
Section Summary: Confirmed COVID-19 cases have been higher in regions with cooler temperatures. However, more recently large-scale community spread has also been established in countries with warmer temperatures. It is unclear if the association with cooler temperatures has been due to differences in weather or is merely a coincidence due to where the outbreak began and how it spread via international travel.
Though there have been many preprints claiming to establish a link between COVID-19 and weather conditions, most do some version of the same analysis. They look at where COVID-19 was spreading the earliest, notice that those places have had relatively cool weather during the period of early spread (i.e. during winter) and suggest that COVID-19 prefers to spread during cold weather. In addition, many of these papers looked COVID-19’s spread through no later than mid-March.
If you look at where the pandemic was in early March, it is certainly true that most cases were occurring in a relatively cool Northern latitude band that included China, Europe, and the United States.
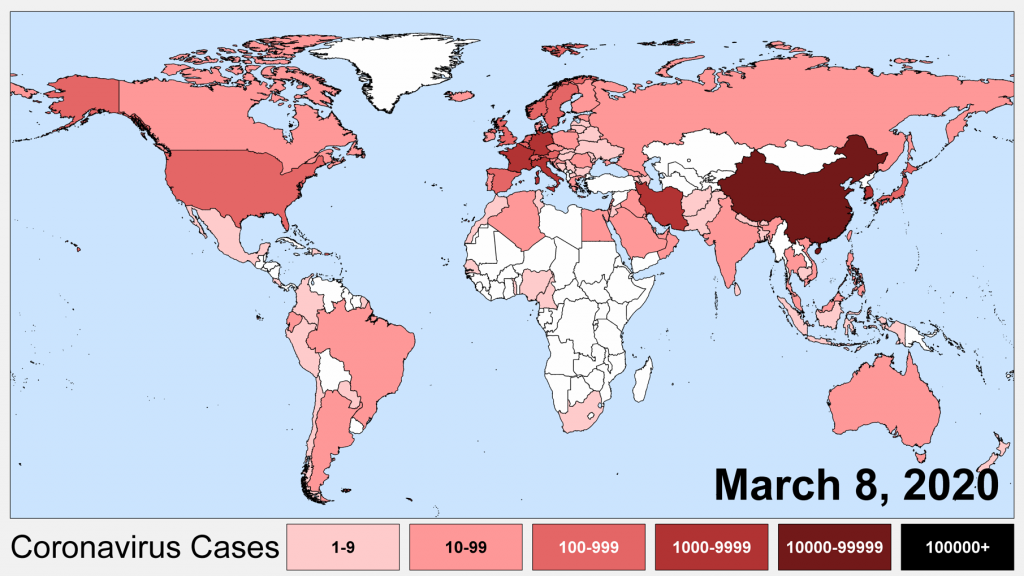
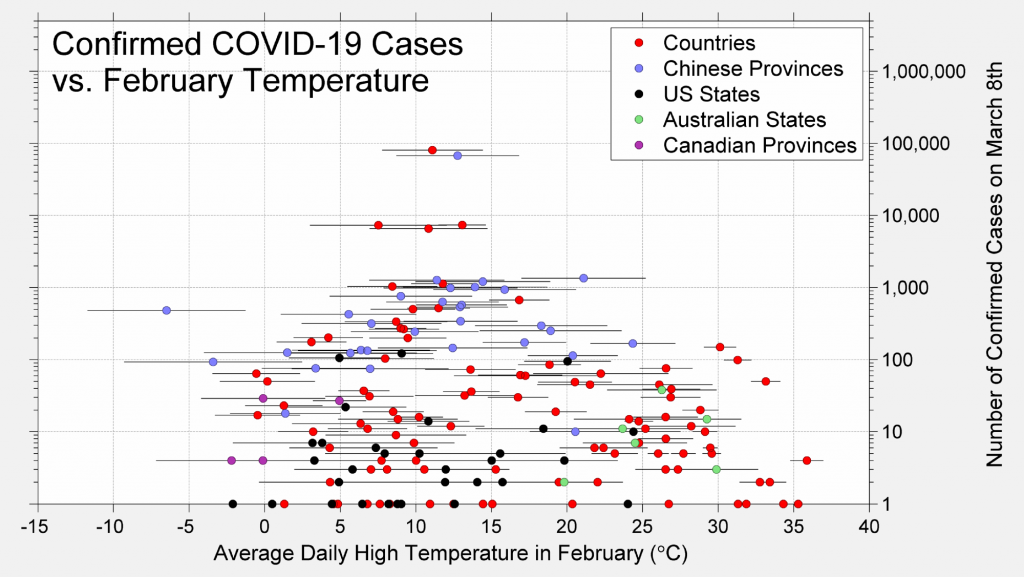
The highest concentration of cases in early March mostly occurred in regions where average high temperatures in February had been between 5 and 15 °C (40 and 60 °F).
Unfortunately, correlation is not necessarily the same thing as causation. The international spread of a novel pathogen is going to be linked to any number of factors, but patterns of international travel will naturally play a large role. After starting in China, it should not be surprising that the disease spread to neighboring countries (e.g. South Korea, Singapore) and to parts of the world with a high volume of international air travel (including Europe and the United States). By contrast, regions with less international travel, such as Africa and South America might reasonably be expected to see a later introduction of the virus. Hence, the early spread of COVID-19 to Europe and North America could plausibly have been coincidental as a result of the patterns of international travel.
Now that more time has passed, the virus has spread more widely. Though many of the largest outbreaks remain in a Northern latitude band, local epidemics are now present in all regions of the world and hence have not been tightly constrained to any single climate. In particular, significant outbreaks have been established in countries like Brazil, Peru, and India, with relatively tropical climates.
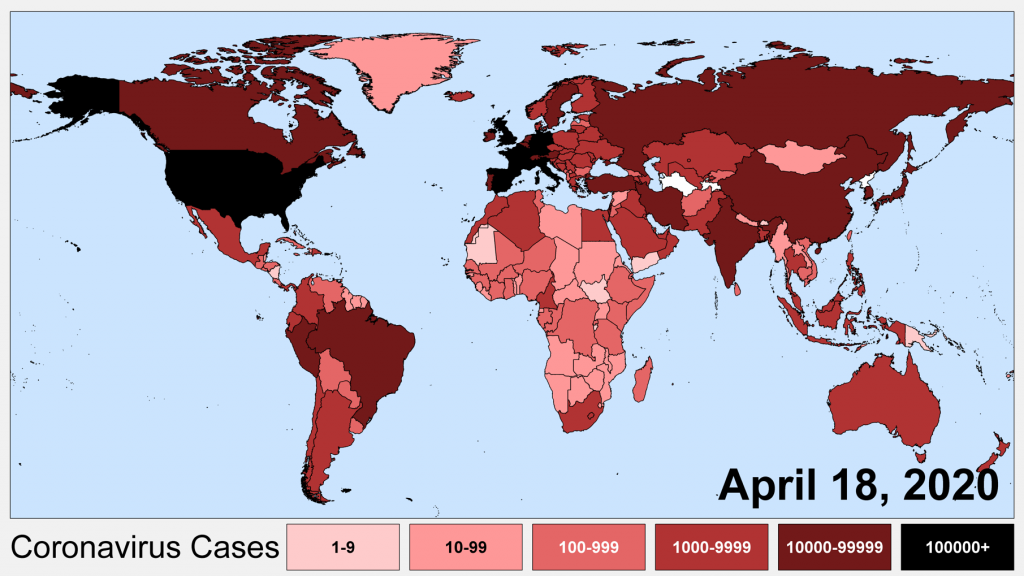
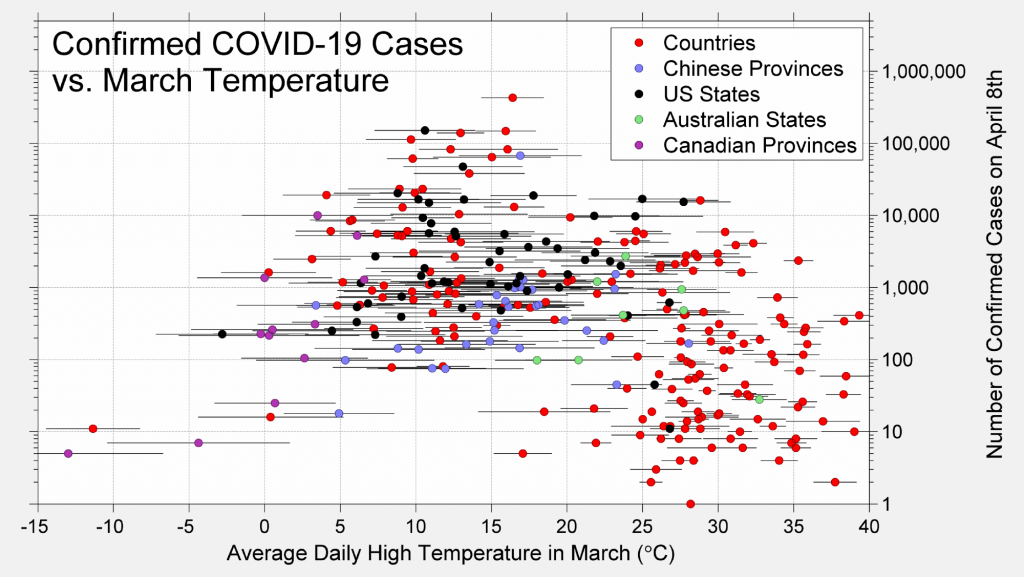
While in mid-March nearly all outbreaks of more than 500 confirmed cases were occurring in countries exhibiting a narrow range of temperatures, by April we now observe that outbreaks of many thousands of cases have occurred in locations with March temperatures ranging from 0 and 35 °C (30 and 95 °F).
It remains true that the highest case counts appear at ambient temperatures around 10 to 20 °C, and there are fewer cases in many warm countries (especially in Africa). However, it is unclear if this reflects an influence of weather or is due to other factors, such as a later introduction of the virus or lower number of tests being conducted in many of the tropical countries.
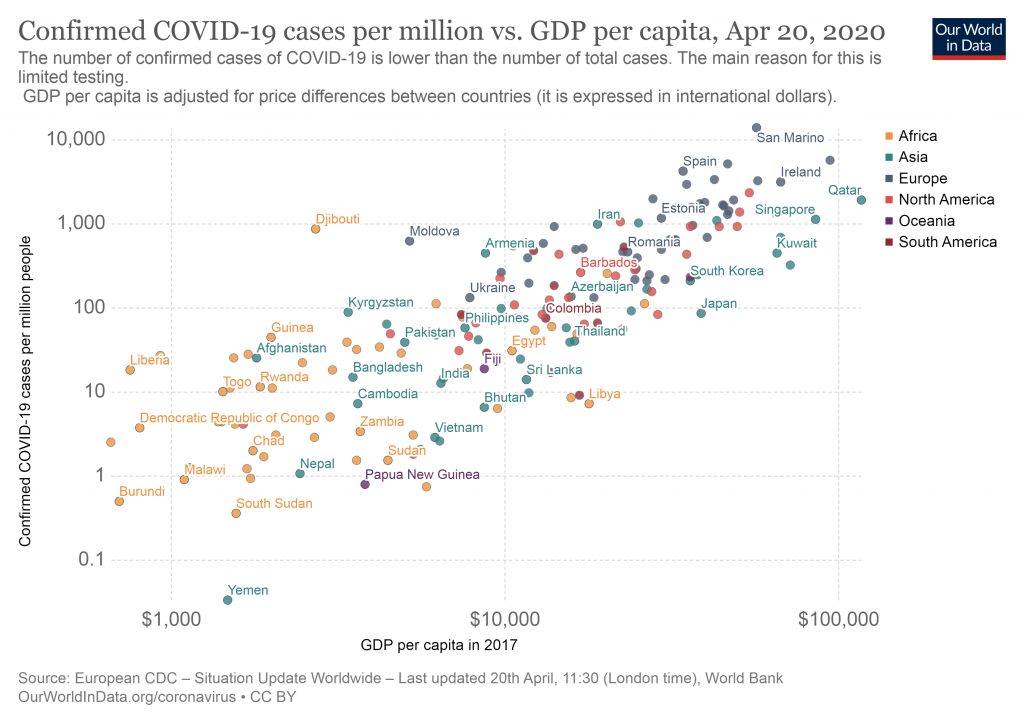
As pointed out by Max Roser and Our World in Data, the number of confirmed cases of COVID-19 per capita appears to track a country’s GDP per capita, with wealthy countries reporting relatively higher numbers of COVID-19 infections In part, this is likely a reflection of both the limited testing in poor countries, and the higher prevalence of international travel in rich countries.
Temperature vs. Growth Rate
Section Summary: Looking at the rate at which COVID-19 has spread allows one to partially correct for differences in outbreak timing and rates of testing. When looking at the rate at spread across a variety of locations, we do not see evidence of a strong role for ambient temperature.
Rather than simply looking at cases totals, a potentially better metric of disease progression is the rate at which the number of confirmed cases is increasing. By looking at the local rate of growth, one can somewhat compensate for differences in when a local epidemic began. Most of the world is currently experiencing an increase in the number of cases between 4 and 10 % per day.
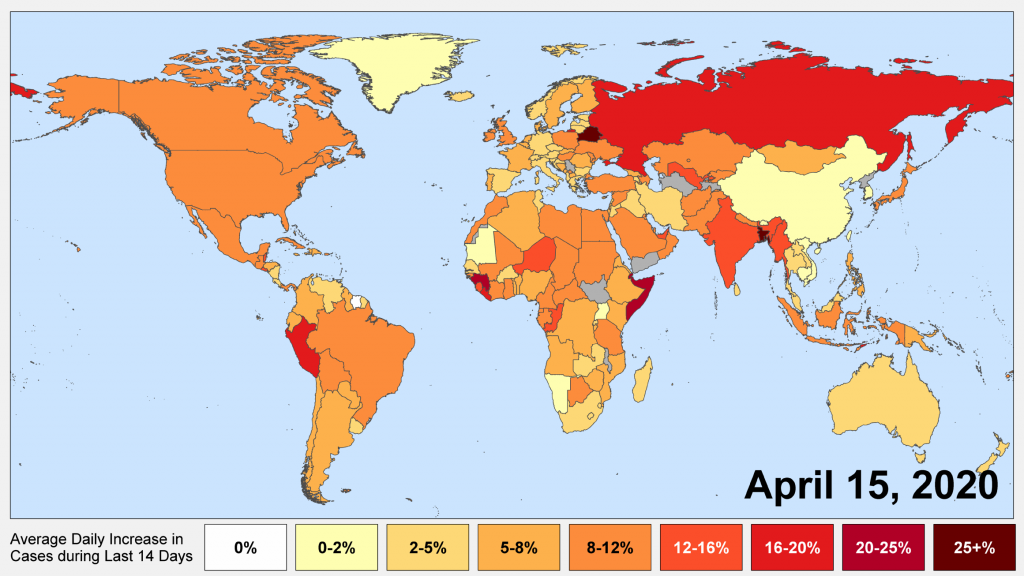
This apparent rate of growth is slower than the 10 to 30% growth many regions reported in the early phases of the epidemic, and is probably affected by the widespread use of social distancing and other control efforts in the present day. There is, currently, relatively little apparent difference in the rate at which confirmed cases are growing in the developed world compared to the developing world.
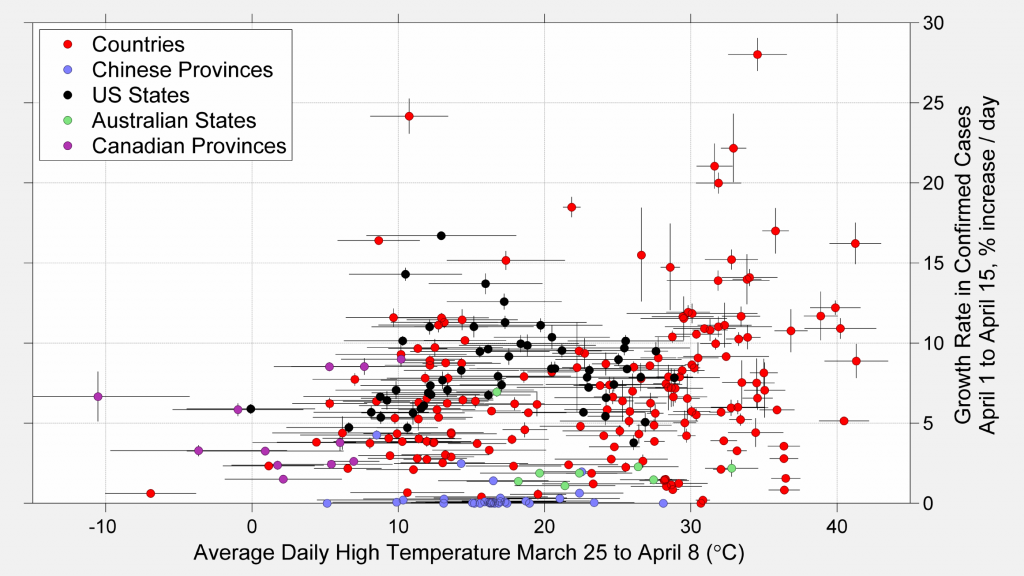
Comparing the recent rate of growth to temperature conditions 1 week earlier, we notice variability among regions, but no evidence that a particular temperature range is closely associated with a faster or slower rate of growth. Notably, a few of the highest rates of growth in the recent period have been associated with warm climates. Warm outdoor temperatures do not appear to present an intrinsic limitation to spread of the coronavirus that causes COVID-19.
Comparing epidemics at similar stages of development
Because epidemics tend to start at different times in different regions and slow down as they progress, a further way of analyzing growth patterns is to restrict our comparison to outbreaks during a similar phase of development.
For the following charts, we have isolated the growth rate of the outbreaks from when each location reported 100 cases to when they reported 1000 cases. This comparison emphasizes a relatively early phase of each epidemic. Initially, these early growth rates are also compared to the average high temperature during an equal window of time shifted 7 days prior. The 7-day delay helps to account for the delay between exposure and diagnosis.
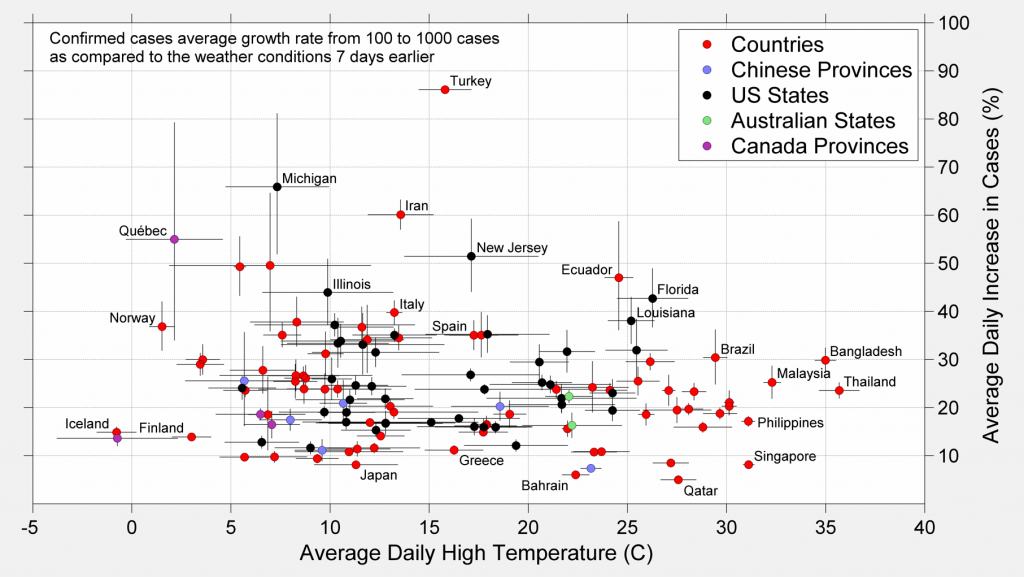
As before there is considerable variation in daily growth rate, which reflects different local conditions and government responses. In particular, some countries have shown much slower apparent growth than other countries.
Significantly though, there has not been a strong relationship between the rate of increase in case counts and the recent daily high temperature. Early in a local epidemic, often before strong countermeasures began, sustained daily growth rates of 15 to 30% can be observed at locations with histories of both warm and cold weather.
Median Daily Growth Rate vs. High Temperature
- -2 to 10 °C: 22% increase per day (3.5 days to double)
- 10 to 25 °C: 21% per day (3.6 days)
- 25 to 37 °C: 22% increase per day (3.5 days
This suggests that outdoor temperature had, at most, only a small influence on the spread of COVID-19 during the early phase of the epidemic. Though not shown, similar results are also found when examining average and low daily temperatures.
Other factors, such as population density and government response, probably play a larger role than outdoor temperature in influencing the spread of COVID-19.
Some authors have chosen to focus on confirmed deaths rather than confirmed cases. The reasoning is that the deaths are less likely to be affected by variations in testing, since deaths are less easily overlooked than mild cases. Repeating the previous analysis for the period when regions reported a growth from 5 to 50 deaths gives similar results.
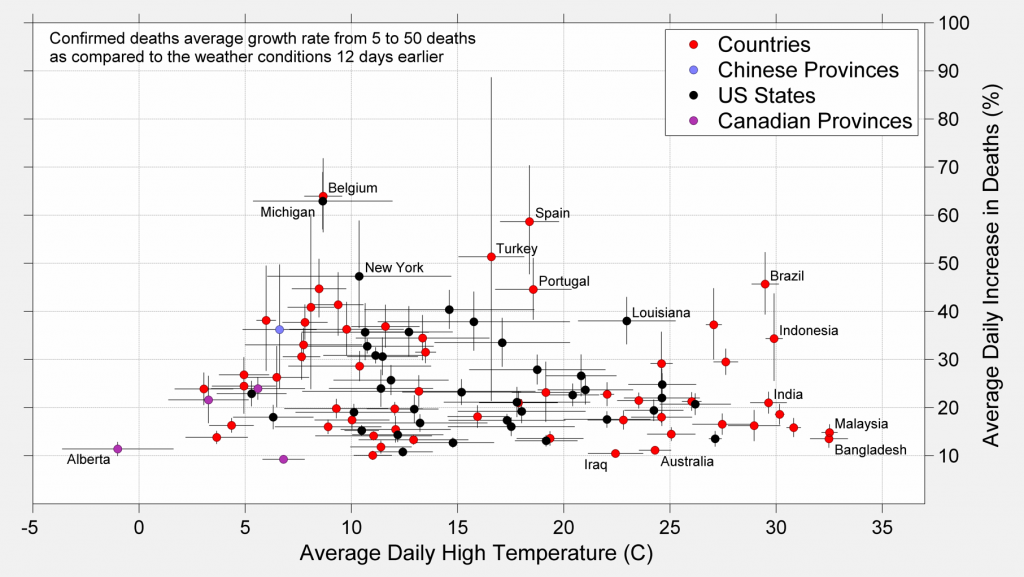
Examining the rise in reported deaths, there is also only a small difference between the median growth rate at 5 to 20 °C, 24% / day and at 20 to 35 °C, 21% / day. However, even at high temperatures the apparent growth rate has been quite substantial and a further indication that weather is unlikely to impose a strong limitation on the spread of COVID-19.
Other Weather Variables
Section summary: An examination of humidity and ultraviolet radiation as alternative weather variables also do not appear to show a strong impact of these variations on the ability of COVID-19 to spread. The ultraviolet flux variable may have a modest impact, but many locations continue to show significant rates of spread even at the higher end of the observed range.
The previous analysis can be repeated for other climate variables. Briefly we present the growth rate vs. relative humidity, absolute humidity, and the average flux of ultraviolet (UV) radiation at the surface. Humidity is generally considered an important factor for the durability of viruses, since many viruses are damaged if they dry out. As before, the growth is measured during the progression for 100 cases to 1000 cases.
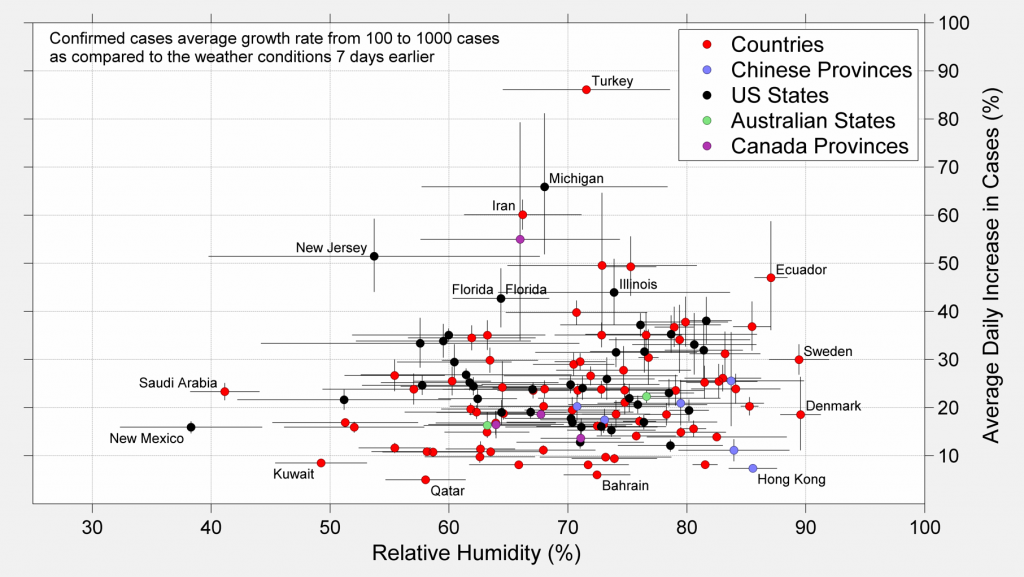
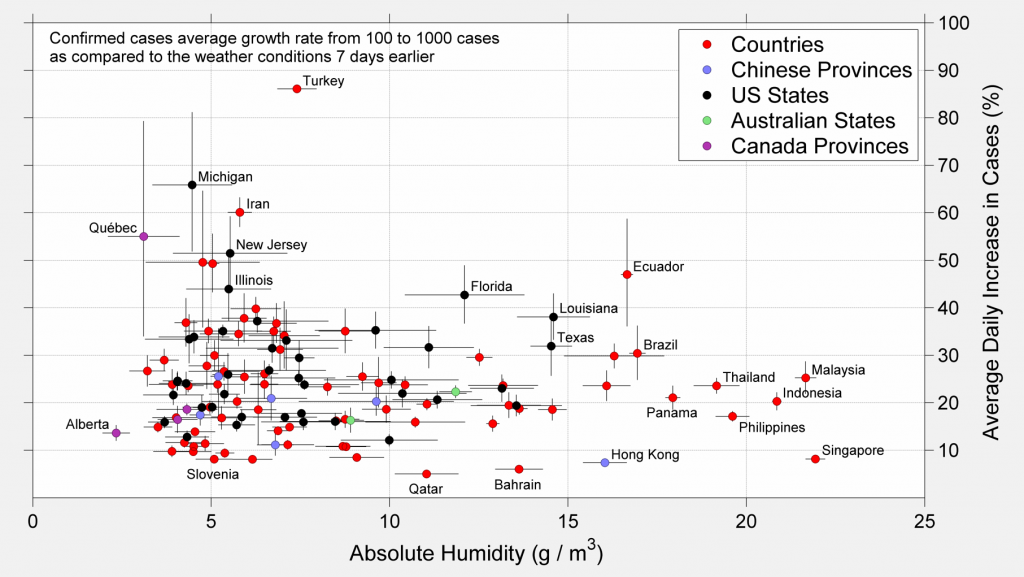
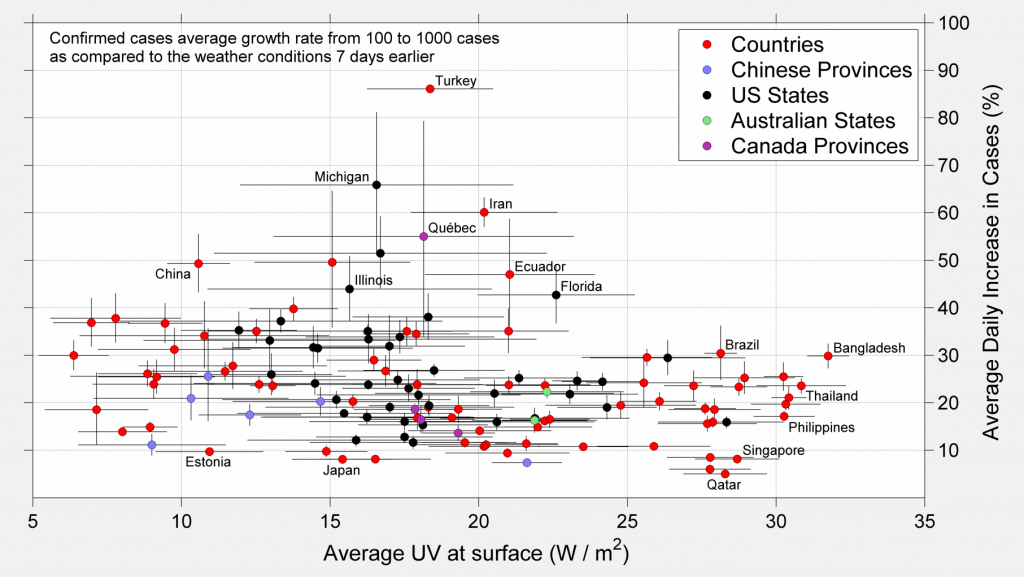
Again, though there is some variations across the range of weather conditions considered, there does not appear to be a strong limitation to spread across the range of environmental conditions considered.
Perhaps the environmental variable with the best suggestion of an impact is UV flux. In that case, locations with an average UV exposure less than 15 W/m2 had a median growth rate of 26% per day (3.0 days to double) during this early phase of the epidemic, while locations with more than 20 W/m2 had a median increase in COVID-19 cases of only 19% per day (3.9 days to double).
Warm weather example
In the discussion of the effect of weather / climate on the spread on COVID-19, it is useful to consider an example of a situation where COVID-19 is spreading under warm conditions.
Perhaps the most telling example is Guayaquil, Ecuador. This port city of 2.7 million people near the equator has an average high temperature between 29° and 32° C (84° and 90° F) year-round. In addition, many residents are too poor to afford air conditioning. Sadly, Ecuador is also home to a severe COVID-19 outbreak.
Officially, Ecuador has 7,466 confirmed cases, 333 confirmed deaths, and 384 probable deaths as of April 13th; however, it is widely acknowledged that the outbreak is much more severe than the official statistics indicate due to a lack of testing. Since the declaration of a public health emergency, Guayaquil has registered 1,878 deaths (most never having been tested for COVID-19) and cemeteries that normally handle ~35 bodies per day are now receiving up to 150. Between April 1st and April 15th, Guayas Province reported nearly 5,000 more deaths than would be expected during the same time frame in a normal year. Moreover, their overwhelmed system is struggling to provide healthcare and dispose of remains. Frightened people are sometimes leaving bodies on the street for days. Obviously, Guayaquil is struggling with severe sustained local transmission despite the equatorial climate.
As the pandemic continues, other warm climate examples of local transmission are also emerging including the slums of Mumbai (average high 32 °C) and Rio de Janeiro (average high 28 °C).
Discussion
At this point in the pandemic, it has become clear that a warm climate, at least up to ~32 °C (90 °F) is not by itself sufficient to prevent local transmission of the coronavirus responsible for COVID-19. Sustained community transmission has already been observed in a variety of countries with warm climates.
Whether a warm or sunny climate might still have a mild effect on slowing transmission is unclear. Some of the above charts suggest that a mild effect is possible. However, the growth rates observed across a variety of climates do not show signs of a strong relationship or limitation across the range of weather conditions that have been observed so far.
One explanation may be that a majority of transmission simply occurs indoors during close interactions with family, friends, and coworkers. A Chinese contact tracing study looking at over 7000 cases with known routes of exposure identified only a single example where the virus was known to have spread during an outdoor contact. It is entirely possible that the lack of evidence of weather effects on the spread of COVID-19 reported above is primarily due to indoor spread under conditions that may be decoupled from the ambient weather.
Under these circumstances, it appears likely that COVID-19 will remain capable of significant spread during warm and sunny conditions, as already evidenced by the serious outbreaks in locations such as Ecuador and Brazil.
One should not expect that the COVID-19 epidemic will simply disappear during summer months. More likely, any change in the evolution of local epidemics will have to be the result of intentional control efforts rather than simply waiting for good weather. In countries that are unable or unwilling to mount effective control measures, the virus may well continue to spread until a sufficient portion of the population has been infected to achieve herd immunity.
These findings also suggest that countries with tropical climates should still be considered to be at risk of wide-scale outbreaks of COVID-19.
Methods
The analysis presented here is based on confirmed cases and confirmed deaths over time as reported by Johns Hopkins University: data portal & time series files. Values through April 19th were used in this analysis.
Temperature, humidity, and UV flux data are compiled from the ERA5 reanalysis dataset. Weather variables are masked to political boundaries using the shapefiles provided by Natural Earth. Representative values for each political territory were constructed using population-weighted averages to better reflect conditions where people actually reside. The Gridded Population of the World Dataset v. 4 data for 2015 is used for this purpose.
In most of the analysis of cases, an offset of seven days was used when comparing case counts to weather conditions. This is motivated by the typical delay of 5 days between exposure and the onset of symptoms, and assuming a further 2 days for diagnosis. In some regions, and early in the pandemic, an even longer delay may be warranted due to the poor availability of testing. However, the conclusions of this report do not appear to be very sensitive to precise choice of delay used.
All analysis and original graphics were produced using Matlab.

